There’s something quietly urgent happening right now. Across the world, millions of people are slowly losing their sharpest memories, their quickest thinking, their clearest sense of self. Dementia is not some distant threat reserved for the very old. It’s a growing, global emergency. Yet here’s the part that most people never hear: a surprising amount of the brain’s fate is in your own hands.
Science in the last two to three years has produced some of its most compelling evidence yet that everyday habits, the kind you can start this week, can genuinely protect your brain. Not just delay decline, but actively improve how your mind works. Let’s dive in.
The Scale of the Problem Is Bigger Than You Think

Let’s start with reality. An estimated 7.2 million Americans over age 65 currently live with Alzheimer’s disease, and that number is expected to nearly double to 13.8 million by 2060. Globally, the picture is equally sobering. These increases reflect more than demographic shifts – they point to a growing public health crisis that requires a new, proactive approach. While chronological age is the strongest known risk factor for cognitive decline, losing cognitive function is not an inevitable part of aging.
That last point matters enormously. In 2024, nearly 12 million family members and unpaid caregivers provided an estimated 19.2 billion hours of care to individuals living with dementia, amounting to a societal cost of more than $413 billion. These numbers aren’t meant to frighten. They’re meant to motivate. Because the same research making those projections is also telling us, with growing confidence, that prevention works.
Up to Nearly Half of Dementia Cases May Be Preventable

Here’s the thing that genuinely surprised me when I first read this: we may already have enough tools to prevent a huge chunk of dementia cases. The 2024 Lancet Commission Report on dementia prevention identified 14 modifiable risk factors that account for approximately 45% of global dementia cases. That is an extraordinary statistic. Nearly half of all cases linked to factors we can actually change.
The Lancet Commission identified risk factors spanning various stages of the life course, including early life factors like education; midlife factors such as hearing loss, traumatic brain injury, hypertension, alcohol misuse, and obesity; and late-life factors including smoking, depression, social isolation, physical inactivity, diabetes, and exposure to air pollution. The message from the world’s leading dementia researchers couldn’t be clearer: this is a problem we can act on, not just observe.
Exercise Is One of the Most Powerful Things You Can Do

I know it sounds too simple. But the evidence for physical activity is genuinely remarkable. Physical activity increases brain-derived neurotrophic factor, which supports hippocampal growth, while also improving blood flow and reducing inflammation. Think of it like fertilizer for your brain. The hippocampus is the region most critical to memory formation, and regular exercise literally helps it grow.
The Alzheimer’s Association’s U.S. POINTER study revealed that lifestyle changes can significantly improve cognitive function in older adults at risk for cognitive decline and dementia. The two-year, multi-site randomized clinical trial tested two lifestyle interventions among a diverse group of 2,111 older adults across five U.S. academic centers and health care systems. Trial participants in the structured intervention showed greater improvement on global cognition compared to the self-guided intervention, protecting cognition from normal age-related decline for up to two years. Two years of structured healthy habits. Real, measurable, cognitive protection.
What You Eat Genuinely Shapes Your Brain

The Mediterranean diet keeps showing up in research for good reason. The Mediterranean diet – characterized by high consumption of fruits, vegetables, whole grains, fish, and olive oil – has been widely recognized for its cardiovascular benefits and may also reduce the risk of cognitive decline and dementia. A comprehensive meta-analysis found a roughly 30% reduction in the incidence of Alzheimer’s disease among those who adhered closely to it.
The Mediterranean and MIND dietary patterns show promise for maintaining cognitive function across studies. Multi-domain interventions that effectively combine dietary modifications with lifestyle changes have been shown to delay dementia onset in at-risk older adults. While both diets offer neuroprotection, findings suggest that the MIND diet may provide slightly superior benefits due to its targeted inclusion of neuroprotective nutrients such as berries, leafy greens, and whole grains. Specific micronutrients, including polyphenols, omega-3 fatty acids, and B vitamins, were found to be significantly associated with better cognitive outcomes and lower neuroinflammation.
Sleep Is Not Optional – Your Brain Depends on It

Honestly, sleep might be the most underestimated brain health tool we have. People treat it like a luxury. It’s not. Research published in Neurology found that adults who had interrupted sleep in their 30s and 40s were more likely to perform worse on cognitive function tests a decade later. A decade later. The damage compounds quietly, long before any symptoms appear.
Even after adjusting for age, sex, education, health, and lifestyle factors, the brains of participants who slept poorly were more atrophied than those who slept well. Compared to those with little trouble sleeping, those with moderate sleep difficulty had brains that were 1.6 years older, while those with the most difficulty had brains 2.6 years older. Research shows that maintaining a regular sleep pattern of at least 7 hours per night enhances working memory and response inhibition in healthy adults. It’s not complicated. It just has to be prioritized.
Loneliness Is a Serious Brain Health Risk

This one genuinely shocks people. Loneliness isn’t just an emotional experience. It’s a physiological threat to your brain. A large-scale analysis examining data from more than 600,000 participants across 21 longitudinal cohorts found that loneliness increased the risk for dementia at a magnitude similar to the impact of being physically inactive or smoking. Specifically, loneliness increased the risk for Alzheimer’s by 14%, vascular dementia by 17%, and cognitive impairment by 12%.
Socially isolated individuals showed lower gray matter volumes in temporal, frontal, and hippocampal regions, and this structural difference partly mediated the association between social isolation and cognitive function at follow-up. The brain, it turns out, is a deeply social organ. Studies have confirmed an association between loneliness, social isolation, and reduced cognitive function in older adults across multiple cognitive domains, as well as a heightened risk of dementia. Staying connected isn’t just good for your mood. It may literally preserve your mind.
Mental Stimulation Builds a Protective Reserve

There’s a concept researchers call “cognitive reserve,” and it’s one of the most fascinating ideas in brain science. Think of it as a buffer – the more you’ve built up through learning and mental activity, the more brain damage your mind can quietly absorb before symptoms start showing. Regular social and cognitive engagement promotes neuroplasticity and mental resilience.
The U.S. POINTER study’s lifestyle interventions both focused on physical exercise, nutrition, cognitive challenge, and social engagement, as well as heart health monitoring, all working together as a system rather than isolated fixes. Reading, puzzles, learning new skills, even picking up a musical instrument – these aren’t just hobbies. Older adults who regularly listen to or play music appear to have significantly lower risks of dementia and cognitive decline. There’s no shortage of enjoyable ways to keep your brain challenged.
Your Heart Health and Your Brain Health Are the Same Thing
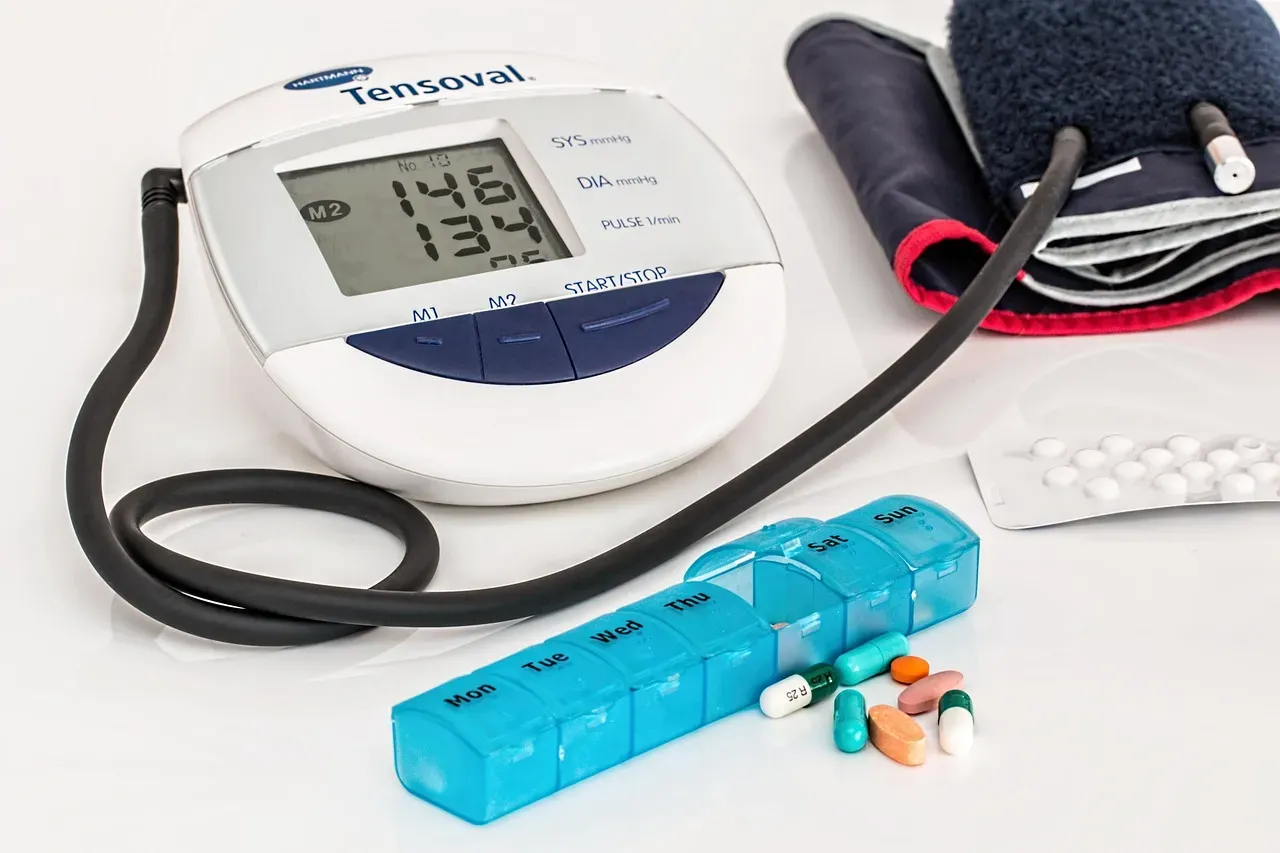
People often treat the heart and brain as separate systems. They’re not. What damages one tends to damage the other. Healthy dietary patterns like the Mediterranean and DASH diets can lower oxidative stress and improve insulin sensitivity, as well as risks of cardiovascular disease. All of this flows upstream to the brain.
Vascular health directly shapes cognitive health. High blood pressure, unmanaged diabetes, and high cholesterol don’t just harm your arteries. They erode brain tissue over time. Getting ample physical activity, eating a healthy diet rich in leafy greens, berries, whole grains, legumes, nuts, and fish, challenging your brain to learn new things, and addressing cardiovascular and metabolic risk factors regularly with your healthcare provider – including high blood pressure, cholesterol, and blood sugar – are all part of a coherent brain health strategy. It’s all connected.
Stress Management Is Not Just Wellness Fluff
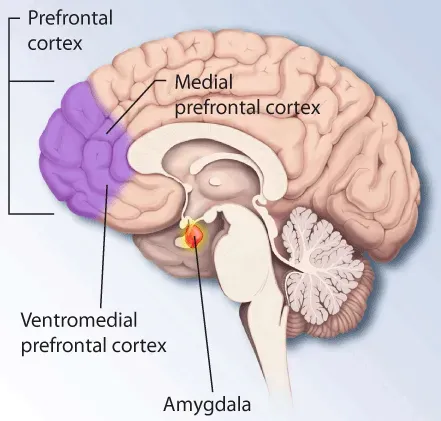
Let’s be real – stress reduction advice often sounds vague. Meditate more. Breathe deeply. Sure. But the actual science behind it is serious. Chronic stress floods the brain with cortisol, and sustained cortisol exposure causes measurable damage to memory structures. Neurobiological changes associated with loneliness and psychological stress include cortisol secretion and brain volume alterations in white and grey matter and the hippocampus.
Mindfulness and relaxation practices aren’t just about feeling calmer in the moment. They create structural and chemical changes in how the brain regulates itself. Poverty, limited healthcare access, and educational disparities heighten cognitive risk, while environmental exposure, such as air pollution, toxins, and social isolation, further contribute – making it clear that promoting healthier habits, including stress-reducing practices, is essential. Managing stress is brain maintenance. Full stop.
No Single Change Is Enough – The Combination Is the Key

Here’s the most important finding from all of this research, and it often gets lost in the headlines. No single habit is a silver bullet. The real power comes from stacking healthy changes together. Both structured and self-guided lifestyle interventions in the U.S. POINTER trial led to cognitive improvements, with the structured program showing greater gains in global cognition. The structured program worked because it combined everything – exercise, diet, cognitive engagement, and cardiovascular monitoring – all at once.
A lifestyle program focusing on improved nutrition, physical exercise, cognitive engagement, and health monitoring improved thinking and memory over two years. The results present a compelling case for investments in preventive brain health programs targeting nutrition, physical exercise, cognitive stimulation, and cardiovascular wellness. The U.S. POINTER trial is the first large-scale trial to demonstrate that accessible, sustainable lifestyle changes can protect cognitive function in diverse communities across the United States. That’s not a small thing. That’s a landmark result, and it belongs in every conversation about how we age.
Conclusion: Your Brain’s Future Isn’t Fixed

The evidence is now clearer than at any point in medical history. Brain decline is not simply fate. It is, to a remarkable degree, a process shaped by choices made across a lifetime. Sleep more consistently. Move your body. Eat foods that protect your neurons. Stay socially engaged. Keep learning. Manage your cardiovascular health. Reduce chronic stress.
None of these changes require expensive treatments or a perfect lifestyle. They require intention. Participants in the U.S. POINTER study changed their behavior over a two-year period and found that their cognitive function scores were on par with people one or two years younger than themselves. That might not sound dramatic. It actually is.
The question worth sitting with isn’t whether these changes work. The research says they do. The question is: which one will you start with today?

