Most of us go through life treating the brain like it will just take care of itself. We sleep badly, eat whatever is quick, skip the gym, and wonder why we feel foggy by noon. The truth is, the choices you make every single day are quietly shaping your cognitive future. And here’s the part that might surprise you – science is increasingly showing that small, consistent habit changes can make a genuine, measurable difference to how your brain ages.
We are in 2026, and the research behind brain health has never been more compelling or more actionable. From landmark clinical trials to sweeping meta-analyses, the evidence keeps pointing in the same direction. Let’s dive in.
1. The Scale of the Problem Is Bigger Than Most People Realize
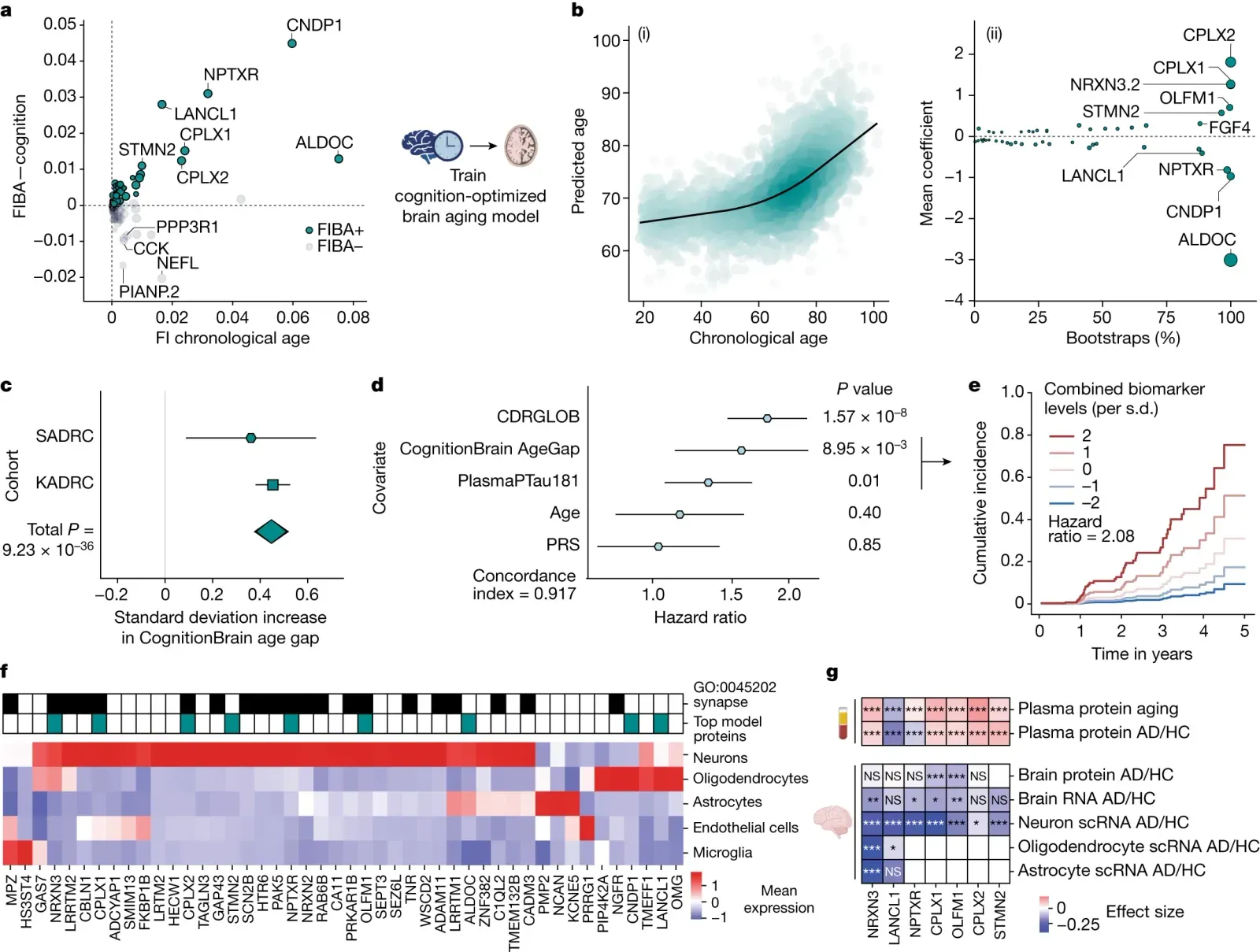
Let’s start with a number that honestly stops you in your tracks. The 2024 Lancet Commission Report on dementia prevention has identified 14 modifiable risk factors that account for approximately 45% of global dementia cases. That means nearly half of all dementia cases could potentially be influenced by things we actually have some control over. That is not a small thing.
The World Health Organization estimates that about 55 million people worldwide currently live with dementia, with close to 10 million new cases every year. The 2024 Lancet Commission Report underscores the need for a global perspective, recognizing that dementia is shaped not only by genetics but also by socioeconomic, environmental, and lifestyle factors. Honestly, that changes the entire conversation.
2. Lifestyle Changes Can Actually Improve Your Cognition – It Is Proven

Here’s the thing – we are not talking about vague wellness advice. We’re talking about hard clinical data. The Alzheimer’s Association U.S. Study to Protect Brain Health Through Lifestyle Intervention to Reduce Risk (U.S. POINTER), a two-year, multi-site clinical trial, found that both structured and self-guided lifestyle interventions improved cognition in older adults at risk of cognitive decline.
The two-year, multi-site randomized clinical trial tested two lifestyle interventions among a diverse group of 2,111 older adults across five U.S. academic centers and health care systems. U.S. POINTER is the first large-scale, randomized controlled clinical trial to demonstrate that an accessible and sustainable healthy lifestyle intervention can protect cognitive function in diverse populations in communities across the United States. That is a landmark finding. Full stop.
3. Regular Exercise Is One of the Most Powerful Tools You Have

I think people underestimate just how directly physical movement connects to brain function. It is not just about heart health or weight. A lifestyle program focusing on things like improved nutrition, physical exercise, cognitive engagement, and health monitoring improved thinking and memory over two years, with results presenting a compelling case for investments in preventive brain health programs targeting nutrition, physical exercise, cognitive stimulation, and cardiovascular wellness.
Data from the Finnish Geriatric Intervention Study to Protect Cognitive Impairment and Disability (FINGER) supports the view that structured brain-healthy habits can improve cognition as we age, with a recently reported decrease in the incidence of overall dementia by approximately 13% across multiple studies, pointing to the potential benefits of lifestyle changes. Think of exercise like a maintenance contract for your brain. Skip it long enough, and things start to break down.
4. What You Eat Shapes How Well You Think

Diet is probably the most underappreciated brain health lever most of us have access to every single day. The Mediterranean diet, characterized by high consumption of fruits, vegetables, whole grains, fish, and olive oil, has been widely recognized for its cardiovascular benefits and may also reduce the risk of cognitive decline and dementia. Findings from a comprehensive meta-analysis provide robust evidence supporting the protective role of the Mediterranean diet in reducing the risk of cognitive decline, dementia, and Alzheimer’s disease.
Research on Mediterranean diet adherence and Alzheimer’s disease incidence has found a 30% reduction in the incidence of Alzheimer’s disease among those following this dietary pattern. That is not a trivial number. It’s worth noting, too, that people following a more Mediterranean-style diet showed a lower risk of developing dementia and slower cognitive decline, according to research from Brigham and Women’s Hospital. Swapping ultra-processed snacks for olive oil and leafy greens might literally be one of the most intelligent decisions you make all week.
5. Sleep Is Not a Luxury – It Is Brain Maintenance

We live in a culture that glorifies being busy and getting by on minimal sleep. It is a bad deal for your brain. Over a three-year follow-up period, individuals with chronic sleep deprivation, defined as fewer than six hours per night, demonstrated significantly greater declines in multiple cognitive domains compared to those with adequate sleep. Worse still, short sleepers exhibited the steepest deterioration in global cognition, memory, executive function, and working memory, with performance gaps widening steadily over time.
Research shows that sleep helps the brain conduct important housekeeping, such as clearing out potentially dangerous beta-amyloid proteins – the same proteins that, in Alzheimer’s disease, form in clusters called plaques that worsen cognitive function. Maintaining a regular sleep pattern of at least seven hours per night enhances working memory and response inhibition in healthy adults. So no, “I’ll sleep when I’m dead” is not a winning strategy.
6. Loneliness and Social Isolation Are Serious Risk Factors

This one surprises people. You might not think of your social life as a brain health strategy, but the data is striking. A study analyzing data from more than 600,000 participants across 21 longitudinal cohorts found that loneliness increased the risk for dementia at a magnitude similar to the impact of being physically inactive or smoking. Specifically, loneliness increased the risk for Alzheimer’s by 14%, vascular dementia by 17%, and cognitive impairment by 12%.
Studies have shown there is an association between loneliness, social isolation, and reduced cognitive function in older adults across multiple cognitive domains, as well as a heightened risk of dementia, with numerous changes to underlying neural biomechanisms including cortisol secretion and brain volume alterations, including in the hippocampus. It is a bit like leaving a powerful computer running constantly in a cold, empty room with no input. The hardware starts to degrade faster than it should.
7. Challenging Your Brain Builds a Buffer Against Decline

There is a concept in neuroscience called cognitive reserve, and it matters enormously. Think of it like a savings account for your brain. The more you deposit through learning, puzzles, reading, and new experiences, the more you have to draw on if disease begins. As dementia is multifaceted and complex, the research community acknowledges that risk reduction strategies are not one-size-fits-all. NIH-funded researchers found that cognitive training conferred a greater degree of protection from dementia for individuals with greater access to education and health care.
Scientists found that cognitive training conferred a greater degree of protection from dementia for individuals with greater access to education and health care. What this tells us is that consistently stimulating the brain throughout your life is not just a nice hobby. It is an actual protective strategy. Learning a new language, picking up an instrument, even doing a challenging crossword – it all contributes.
8. Your Heart Health Is Your Brain Health
Here is a connection that doesn’t get nearly enough attention outside of medical circles. The brain is extremely dependent on blood flow, and anything that damages your cardiovascular system also damages your cognitive capacity. Addressing cardiovascular and metabolic risk factors regularly with your healthcare provider, including high blood pressure, cholesterol, and blood sugar, is as critical as getting ample physical activity and eating a healthy diet rich in leafy greens, berries, whole grains, legumes, nuts, and fish.
The Lancet Commission identified midlife cardiovascular risk factors including hypertension, alcohol misuse, and obesity as modifiable risk factors linked to dementia across various stages of the life course. It’s hard to say for sure exactly how much of your brain health comes down to blood pressure control alone, but the relationship is strong and consistent across study after study. Managing your blood pressure in midlife might be one of the highest-value investments you ever make.
9. Mindfulness and Stress Reduction Are Not Just Trends

Chronic stress does tangible damage to the brain. The science here is clearer than many people realize. Chronic stress triggers pro-inflammatory cytokine release, neurotransmitter imbalance, and impaired synaptic plasticity, leading to neuronal damage. It also disrupts glymphatic clearance, promoting neurotoxic metabolite buildup, and neuroinflammation and neurotransmitter imbalance can reinforce each other in a vicious cycle that accelerates cognitive deterioration.
Stress reduction practices including mindfulness, relaxation techniques, and even regular time in nature have been shown in recent research to improve attention, emotional regulation, and overall cognitive performance. Environmental exposures such as toxins and social isolation further contribute to dementia risk, while promoting healthier habits including cognitive engagement is essential. The evidence for stress management as a brain health tool is solid, even if a quiet morning routine feels embarrassingly simple compared to pharmaceutical interventions.
10. No Single Change Is Enough – The Combination Is What Wins

Here’s the most important takeaway from all of this research. There is no magic bullet. Not one habit, supplement, or routine that single-handedly protects your brain. What consistently works is the combination. Both interventions in the U.S. POINTER trial focused on physical exercise, nutrition, cognitive challenge and social engagement, and heart health monitoring, and both led to measurable improvements.
The Mediterranean and MIND dietary patterns show promise for maintaining cognitive function across studies, while multi-domain interventions like FINGER effectively combine dietary modifications with lifestyle changes to delay dementia onset in at-risk older adults. Scientists think lifestyle changes that improve cognition and reduce brain age are likely to delay dementia, including Alzheimer’s, and the Alzheimer’s Association is planning to invest another $40 million over four years to implement what they have learned from the POINTER trial. That level of institutional investment says everything about how seriously the scientific community now takes these lifestyle interventions.
The Bottom Line: Your Habits Are Writing Your Brain’s Future

The research from 2023 through 2025 keeps arriving at the same conclusion. Brain health is not fixed. It is not purely genetic. It is, to a remarkable degree, shaped by the choices you repeat every single day. Exercise more. Sleep consistently. Eat a diet rich in whole foods. Stay connected with other people. Keep learning. Manage your blood pressure. Reduce chronic stress.
None of these are revolutionary ideas. What is revolutionary is the quality of evidence now backing them up. The 2024 updated report on dementia prevention, intervention, and care by the Lancet Standing Commission suggests that if 14 modifiable risk factors were eliminated through both individual lifestyle changes and population-based policy changes, the number of dementia cases could be reduced by 45%.
We now know, with more certainty than ever before, that the brain is responsive. It adapts. It rewards consistent care. The question is no longer whether these simple changes work – the question is whether you’ll start making them. What would you do differently starting today?

