Think about that for a second. The device you use to scroll through news, order pizza, and set alarms is quietly becoming one of the most powerful health monitoring tools ever created. It sounds like science fiction, but it’s 2026 and this is genuinely happening right now, in real time, in millions of people’s pockets around the world.
The convergence of artificial intelligence, sensor technology, and mobile computing has opened a new era in preventive healthcare. Conditions that once required hospital visits and expensive lab tests are now being flagged during a morning walk or while you sleep. Let’s dive in.
The Scale of the Opportunity Is Hard to Overstate
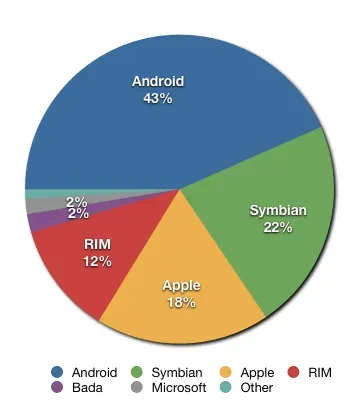
Here’s a stat that puts everything in context. In 2024, roughly nine out of ten adults in the United States said they own a smartphone, according to data from the Pew Research Center. That kind of reach is unprecedented for any medical technology.
No clinical trial, no hospital network, no government screening program has ever had that kind of distribution. When a health detection feature lands on a smartphone update, it reaches more people overnight than most healthcare innovations reach in decades. That’s a genuinely remarkable shift in how medicine can work.
Think of it like this: imagine a diagnostic tool that fits in your back pocket, costs nothing extra, and is already in nearly every home in the country. That’s not a futuristic dream. That’s the starting point for everything that follows.
Heart Rhythm Detection – The Feature That Quietly Started a Revolution
The Apple Watch’s atrial fibrillation history feature has achieved a significant milestone by becoming the first-ever digital health technology to qualify for the FDA’s Medical Device Development Tools program as a class II photoplethysmography analysis software for over-the-counter use. That’s a big deal, even if the wording is dry.
The feature estimates how frequently the user shows signs of the irregular and often rapid heartbeat associated with AFib and derives AFib burden estimates, meaning the overall duration of AFib as a percentage of the total time assessed. What this means in plain English is that your watch is quietly tracking your heart rhythm across the day and week, looking for patterns that no single 30-second ECG could catch.
Atrial fibrillation is a type of irregular heart rhythm where the upper chambers of the heart beat out of sync with the lower chambers. According to the CDC, approximately two percent of people younger than 65 and nine percent of people 65 and older have AFib. Many of them don’t know it until something serious happens.
The Samsung Galaxy Watch Joins the FDA-Cleared Club

Apple wasn’t alone for long. The Samsung Galaxy Watch has also received FDA clearance for irregular heart rhythm notifications in the U.S., expanding the ecosystem of regulated, smartphone-connected cardiac monitoring well beyond a single brand or platform.
This matters because competition in this space pushes innovation faster. When two of the world’s biggest consumer electronics companies are both racing to offer clinically relevant heart monitoring, the technology improves quickly and prices stay accessible. Honestly, the winners here aren’t the tech companies. The winners are patients.
The American College of Cardiology and the European Society of Cardiology have suggested using wearable devices for diagnosis and long-term surveillance of AFib, though they urge caution due to the need for further clinical validation. The science is promising. The clinical guardrails are still catching up, which is a fair and reasonable place to be.
Cardiovascular Disease – Why All of This Urgency Actually Makes Sense

Let’s be real about what’s at stake. The World Health Organization reports that cardiovascular diseases remain the single leading cause of death globally, responsible for roughly 20.5 million deaths every year. That number creates enormous pressure to find smarter, earlier, and more accessible tools for detection.
The absence of specific symptoms in many patients can lead to delayed diagnosis, potentially resulting in clinical consequences, with stroke often being the first noticeable presentation. Timely diagnosis leading to early antithrombotic treatment can prevent this lethal complication. That’s the core argument for smartphone-based detection. Earlier is better. Always.
Timely diagnosis of atrial fibrillation and consequent use of chronic oral anticoagulation in high-risk patients can reduce the risk of stroke. Even in otherwise healthy users, atrial fibrillation may be the first manifestation of other diseases. A device that catches this early could be the difference between a long and healthy life and a life-altering emergency.
Your Voice Might Reveal Whether You Have Diabetes

This one genuinely surprised me when I first came across it. Determining whether a person is diabetic could be as easy as having them speak a few sentences into their smartphone, according to a groundbreaking study from Klick Labs that combines voice technology with artificial intelligence. The study outlines how scientists used six to ten seconds of people’s voice, along with basic health data including age, sex, height, and weight, to create an AI model that can distinguish whether that individual has Type 2 diabetes.
In the study, researchers asked 267 people with and without Type 2 diabetes to record clips of their voice up to six times a day for two weeks, garnering more than 18,000 voice samples. They studied differences in pitch, intensity, jitter, and shimmer. These are changes so subtle the human ear can’t catch them. A machine can.
Using this data, they created an AI model that could detect diabetes with 89 percent accuracy in women and 86 percent accuracy in men. The AI was able to flag voice differences even in people with similar age, sex, and body mass index. It’s worth noting this was a relatively small study requiring further validation. Still, the direction is clear.
Camera-Based Heart Rate Monitoring – Your Phone Sees Your Pulse

Here’s something most people don’t realize their phone can already do. Research published in The Lancet Digital Health in 2023 found that smartphone camera-based photoplethysmography, known as PPG, can reliably estimate heart rate and detect irregular rhythms under controlled conditions. Basically, the camera can detect tiny color changes in your skin caused by blood flow with each heartbeat.
It sounds almost magical. Your phone’s rear camera, pressed gently against a fingertip, picks up changes in light absorption that correspond to your pulse. No clip, no chest strap, no extra hardware. Just the camera that’s already there, doing something entirely new.
The limitations are real. Controlled conditions matter. Motion, lighting, and skin tone can all affect accuracy. But as a first-line screening tool, especially in settings where formal medical equipment is scarce, the potential here is significant and worth watching carefully.
AI-Powered Skin Condition Screening Gets Smarter
In 2024, Google’s Pixel devices expanded their skin condition analysis tool. Originally launched as the Google Health AI dermatology assist feature, it uses image-based machine learning models trained on thousands of dermatology images to help users identify potential skin concerns. You photograph a spot or rash and AI compares it against a large clinical dataset.
This is not a replacement for a dermatologist. Let’s be crystal clear about that. It’s a triage tool. It’s the difference between a worried person waiting months for a specialist appointment and a worried person who gets directed to urgent care within the same week because the app flagged something concerning.
Speed matters enormously in conditions like melanoma. Early-stage skin cancer is highly treatable. Late-stage skin cancer often is not. A tool that nudges someone toward earlier evaluation, even imperfectly, could genuinely save lives at scale.
Cough Analysis – Your Microphone as a Respiratory Sentinel

Cough sound offers the possibility of an accessible, non-invasive, and low-cost disease biomarker, particularly in the era of rapid development of machine learning capabilities in combination with the ubiquity of cellular technology with high-quality recording. Researchers have been building on this idea actively through 2023 and into 2025.
Swaasa is a mobile-based AI application that analyses short cough recordings to identify indicators of respiratory conditions such as asthma, tuberculosis, and COVID-19. With a reported accuracy of over 90 percent, the app offers a non-invasive, quick, and accessible screening method that requires nothing more than a smartphone.
Mobile technologies such as wearables and smartphones enable automated, continuous, noninvasive monitoring and allow the detection of subtle changes in vital signs. Cough can be effectively monitored through mobile technologies as it is not only a symptom of prevalent respiratory diseases such as asthma, lung cancer, and COVID-19 but also a predictor of acute health deterioration. These are screening tools at this stage, not diagnostic ones. Clinical validation is still ongoing.
The Regulatory Framework Is Growing Up Alongside the Technology

One of the most important but least-discussed aspects of this whole story is how the FDA has been evolving its approach. The FDA has cleared multiple mobile health apps for monitoring blood oxygen saturation and heart rhythm, reflecting a genuine regulatory recognition of smartphone-based diagnostics as a legitimate medical category.
The U.S. Food and Drug Administration has qualified the Apple Watch atrial fibrillation history feature as the first digital health technology tool for its Medical Device Development Tools program. Through this program, the Apple Watch AFib history feature can be used as a noninvasive method to collect data for device evaluation in clinical trials on a case-by-case basis.
The regulatory environment still lags behind the pace of innovation, which is honestly unavoidable and probably the right call. Moving fast with medical tools carries real risks. Still, the direction is clear: regulators are building frameworks to accommodate this technology, not block it. That’s an important and encouraging signal for the years ahead.
The Billion-Dollar Healthcare Shift Already in Motion

A 2023 report by McKinsey estimated that digital health technologies, including remote monitoring through smartphones, could generate somewhere between $300 and $450 billion in value annually in the U.S. healthcare system alone. That figure includes cost savings from earlier detection, reduced hospitalizations, and more efficient care delivery.
To put that in perspective, that’s not just a technology story. That’s a fundamental restructuring of how healthcare economics work. When detection moves from hospitals to smartphones, the entire cost structure shifts. Fewer late-stage diagnoses mean fewer expensive emergency interventions. Prevention becomes financially viable in ways it hasn’t been before.
Artificial intelligence and wearable technology are increasingly used in healthcare and hold significant potential for improving the management of diabetes. Wearable devices enable continuous monitoring and real-time data collection, supporting AI-driven personalized interventions. This kind of real-time feedback loop, something that was unimaginable even ten years ago, is now a commercial reality.
Conclusion: The Doctor in Your Pocket Is Getting a Lot Better
What’s happening right now in smartphone health technology isn’t a gimmick or a wellness trend. It’s a genuine structural shift in how diseases get detected, and it’s happening faster than most people realize. Heart rhythm abnormalities, early diabetes signals, respiratory patterns, skin conditions – the list of things your phone can now flag is growing year by year.
The technology still has real limits. Accuracy varies. Clinical validation is still catching up with commercial deployment. And there are important equity questions about who benefits and who gets left behind when health tools are tied to device ownership. These are not small concerns.
But here’s what I think is easy to miss in all the nuance: millions of people will likely catch serious conditions earlier because of these tools, conditions that would have gone unnoticed until a crisis forced them into an emergency room. That’s not a minor footnote. That’s a profound change in human health outcomes. Does your phone already know something about your health that you don’t? That question is less hypothetical with every passing year.